

Revenue Cycle Management

We capture accurate patient details and book appointments to kickstart your revenue cycle.

We verify patient coverage in real time to prevent claim denials before treatment begins.
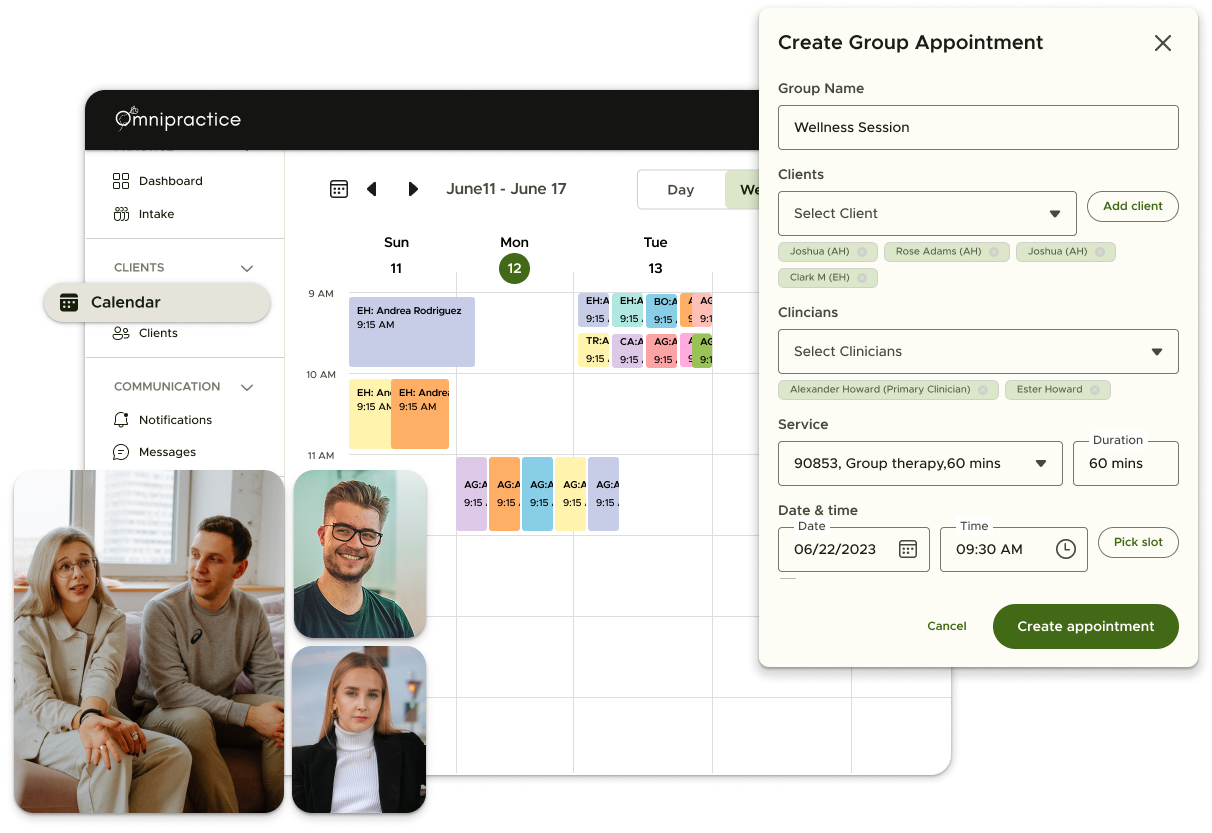
We apply precise CPT and ICD-10 codes to maximize your reimbursement and ensure compliance.
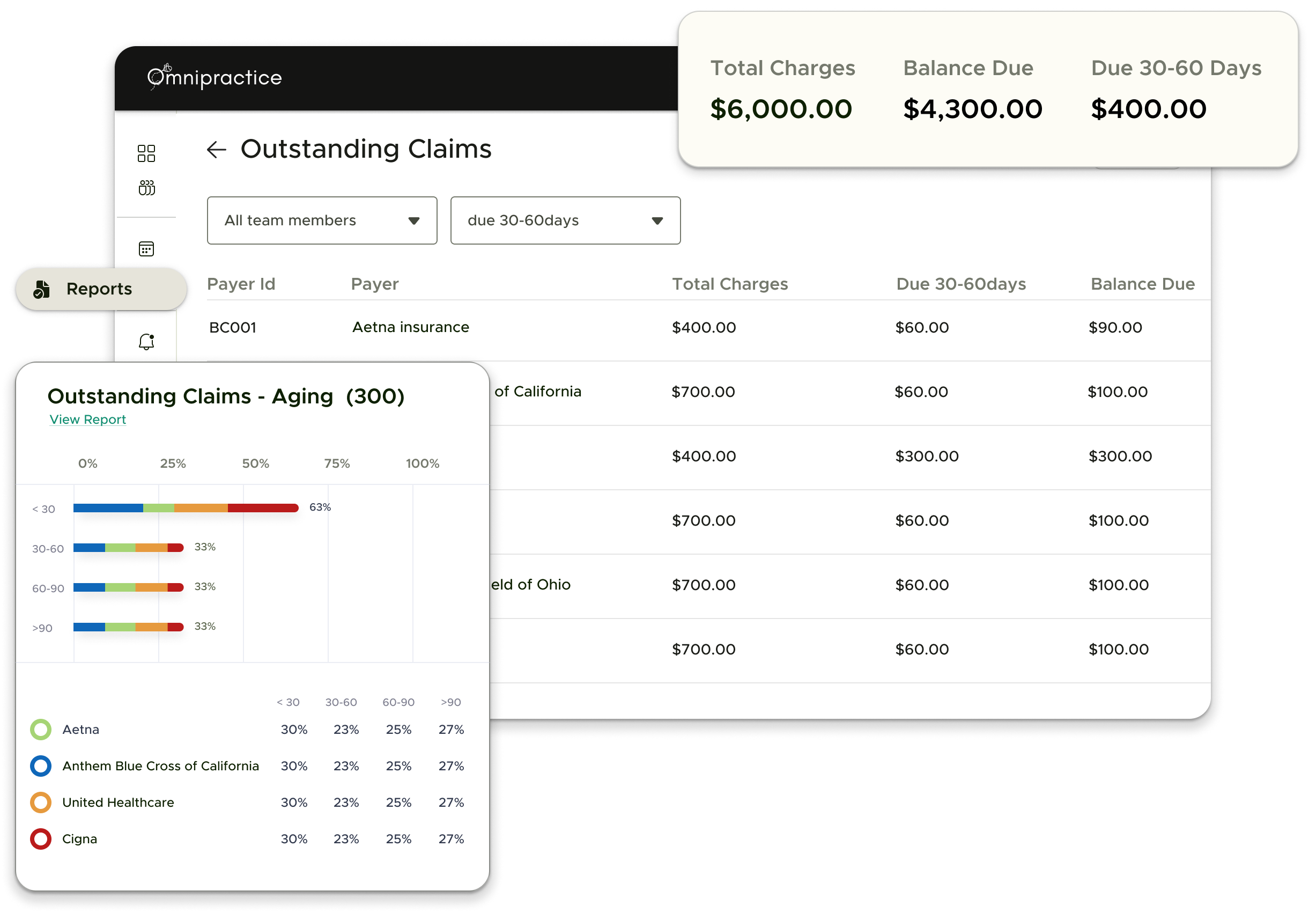
We submit clean claims faster with automated scrubbing to boost your first-pass acceptance rates.

We post payments and reconcile your accounts automatically while tracking every dollar of revenue.
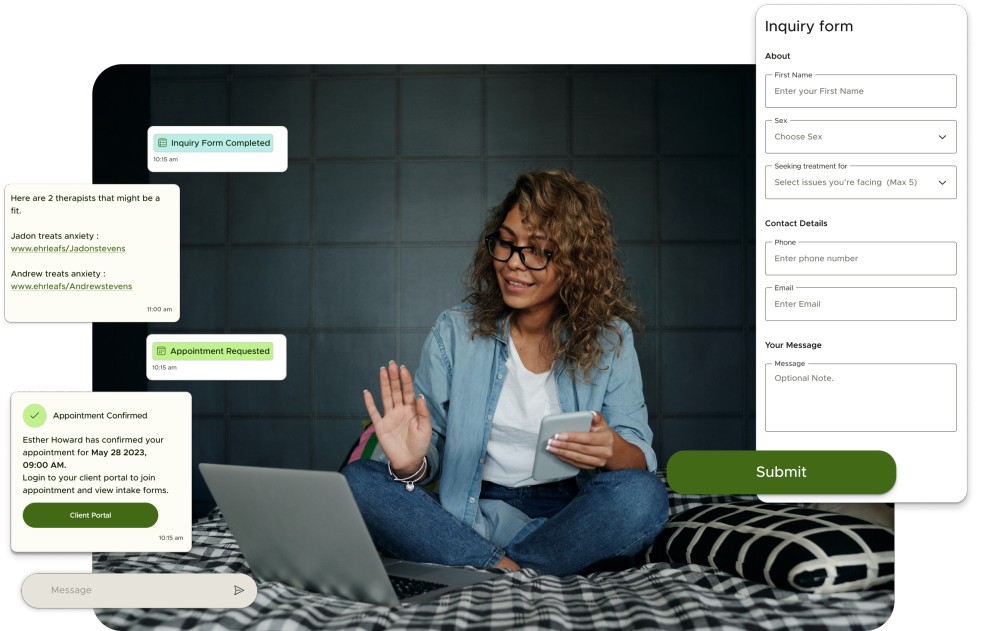
We identify and appeal denied claims quickly using data-driven workflows to recover your revenue.
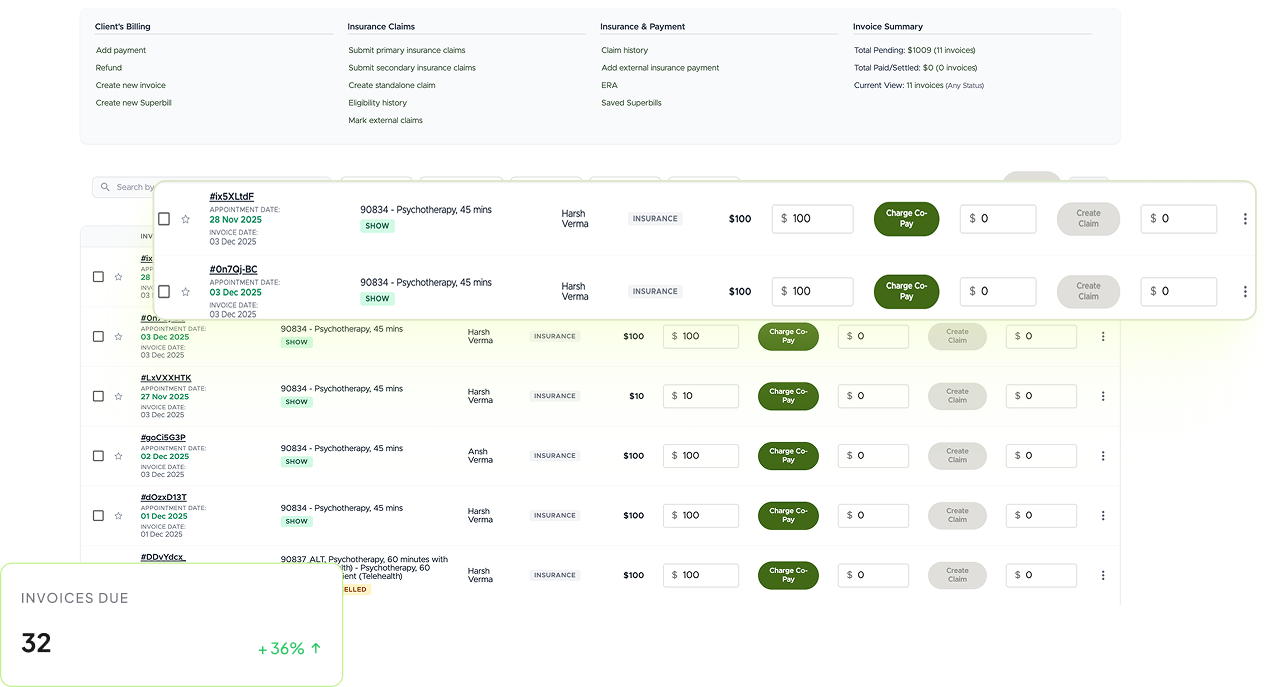
We send clear bills with flexible payment options to improve your collections and patient satisfaction.
Our AI catches missing modifiers, NCCI conflicts, and eligibility gaps before submission — not after a denial wastes 30 days.
→ Industry average: 75–85%
We fix the root cause upstream. The industry average denial rate runs 10–15%. Ours doesn’t.
→ Industry average: 10–15%
Our human team doesn’t let claims age. We follow up, appeal, and escalate until you’re paid.
→ Industry average: 40–65 days
New clients consistently collect more than they were with their previous biller — without seeing more patients.
→ Because you were already leaving it on the table.
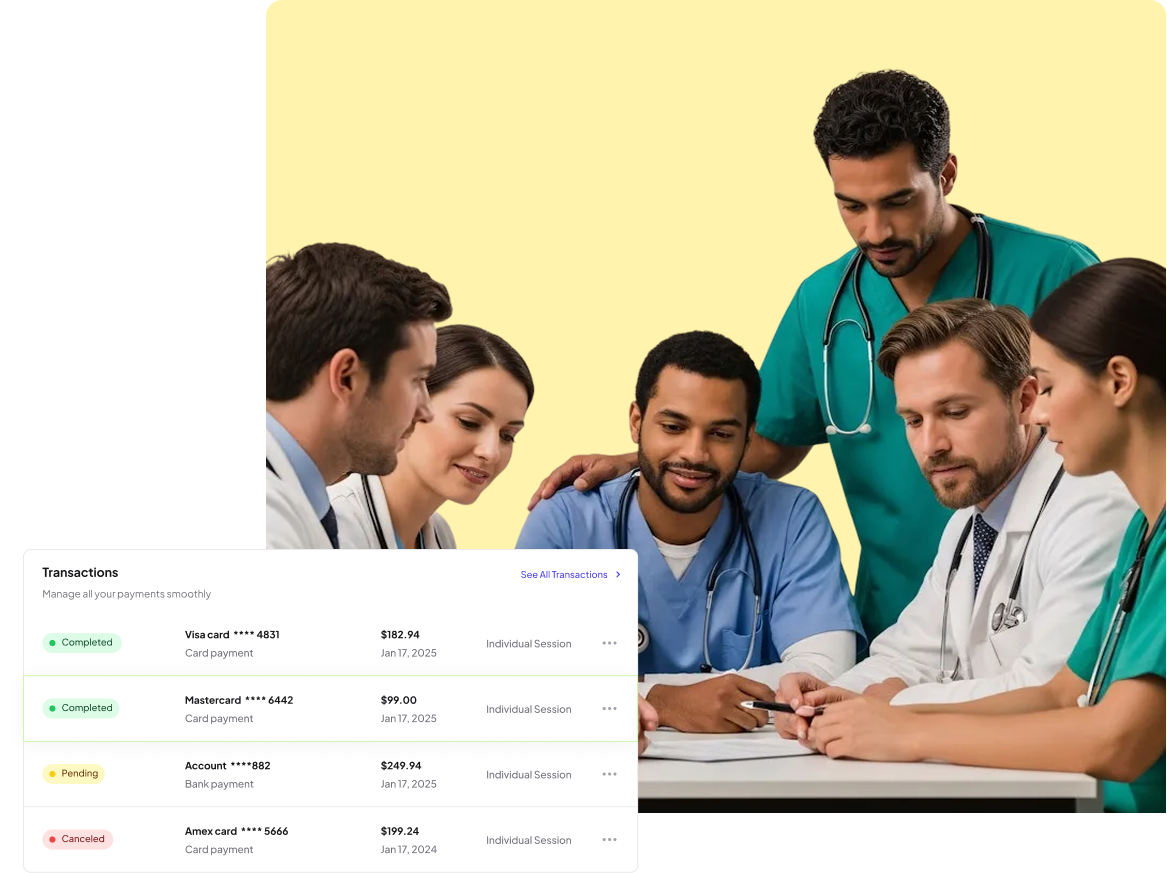






1. Seamless payer coordination for faster, hassle-free claims
2. Complete claim lifecycle management, from submission to payment posting and denial resolution
3. Proactive A/R follow-up to speed up reimbursements and minimize outstanding balances
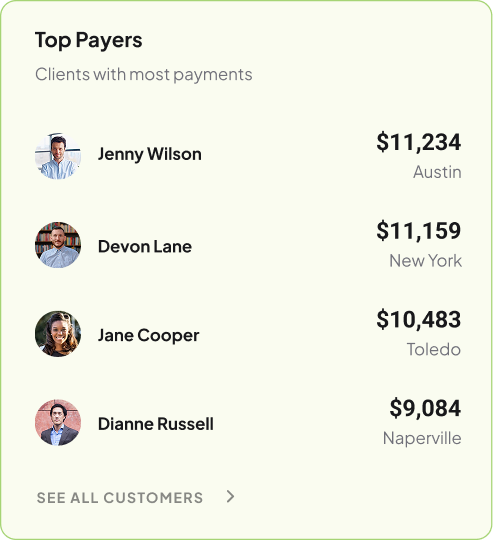
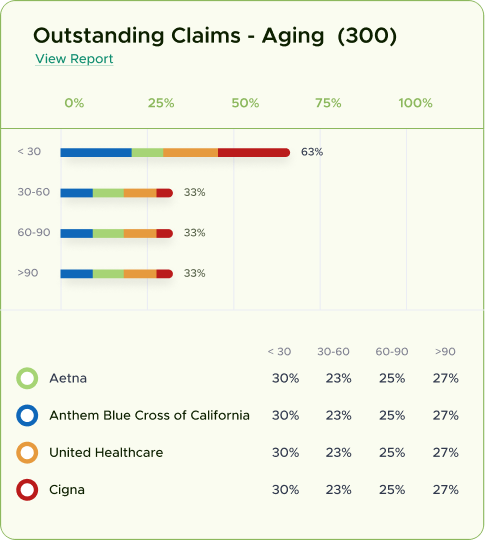
1. Optimized AI workflows that speed up payment
2. Accurate, on-time payment reconciliation with AI
3. Effortless claim submissions with the help of AI





















Call us or
schedule a demo

We audit your last 90 days of claims for free, no obligation.
We connect directly to your EHR and PM system.
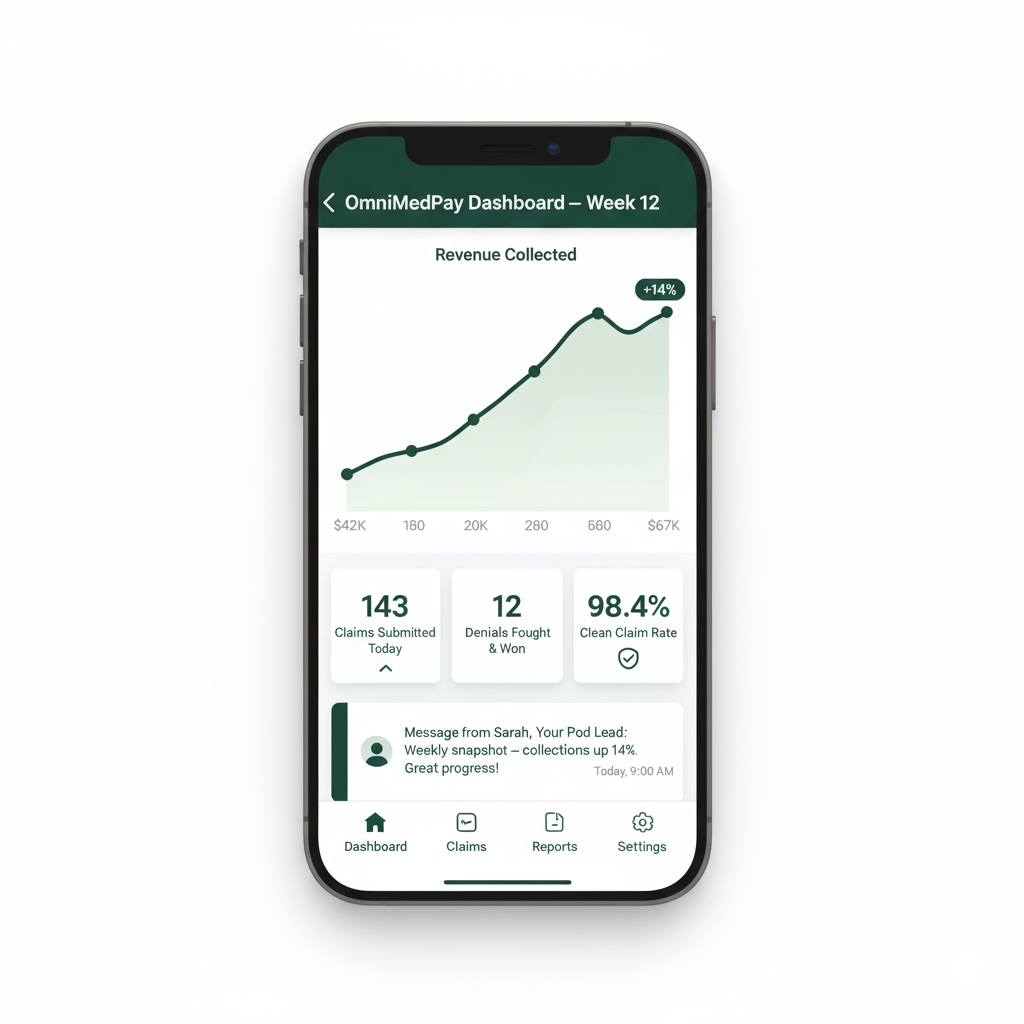
Claims go out daily. Denials get fought. Your dashboard goes live.
We migrate patient data, A/R ledgers, and claim history from your legacy system securely.
Your billers and front-desk staff get trained on scrubbing, posting, and denials immediately.
We configure claim edits, fee schedules, and dashboards to match your reimbursement strategy.
EDI enrollments, ERA setups, and clearinghouse connections — ready to submit claims day one.